Electronic health records were originally introduced to solve one problem: replace paper charts with digital systems. In many ways, that goal has been achieved. Hospitals and clinics now store vast amounts of patient information in centralized EHR platforms.
But digitizing records was only the first step. The real challenge today is making sense of the enormous amount of data these systems contain and extracting decisions that actually move the needle on care quality.
This is where artificial intelligence EHR integration comes in.
Below, we explore what drives the adoption of AI tech, the benefits of AI EHR system, and key use cases with real-world examples already changing the way healthcare organizations operate.
The drivers of AI-enabled EHR market
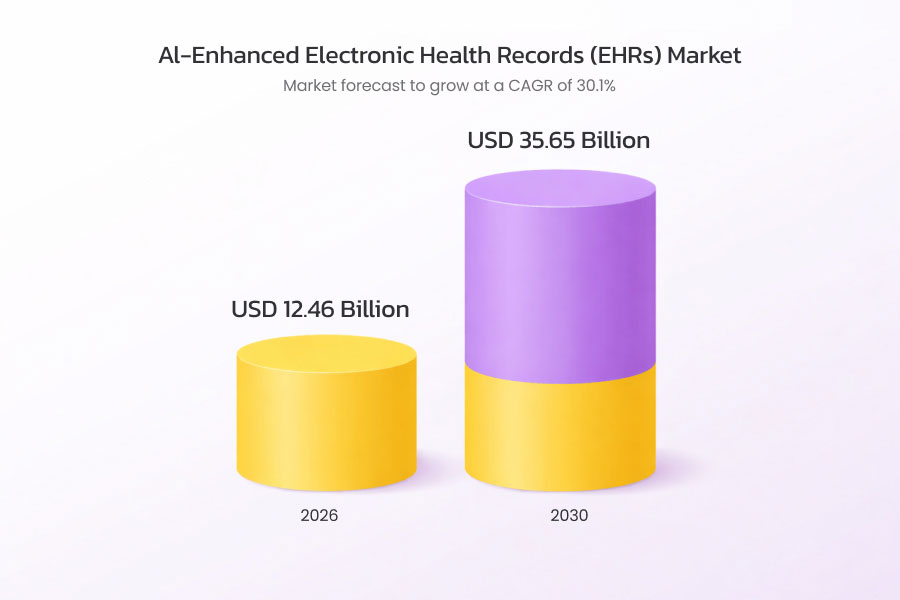
Industry forecasts reveal that the global market for AI-enhanced EHRs is set to skyrocket, with a compound annual growth rate (CAGR) of around 30% over the next decade. This explosive growth is fueled by the urgent need for data-driven healthcare systems and smarter clinical tools that can truly make a difference in patient care.
Geographically, North America currently leads this market, accounting for roughly 41.8% of the global share. This leadership is largely the result of three key advantages:
- a mature healthcare IT infrastructure;
- widespread EHR adoption;
- a strong ecosystem of health-tech companies developing specialized AI ehr software and clinical tools.
Another important factor is data availability. Healthcare organizations in North America have access to massive troves of structured medical data that is a crucial ingredient for training and improving AI algorithms.
Several broader trends are accelerating the adoption of AI and EHR systems.
Rapid digitalization of healthcare systems
Electronic health records have already become a standard component of modern healthcare systems. More than 85% of hospitals in the US now use EHR solutions, reflecting the global shift away from paper-based records. Nearly 67% organizations are already integrate AI in EHRs to unlock deeper insights from medical data.
Explosion of healthcare data
Patient records now include information from multiple sources, including diagnostic imaging, wearable devices, lab tests, and clinical notes. AI healthcare technologies such as machine learning, deep learning, and NLP allow EHR software to process large datasets and uncover patterns that can support clinical decision-making.
Rising administrative burden in healthcare
Another major driver of AI adoption is the growing administrative workload faced by healthcare professionals. Even with the software in place, physicians still would spend a substantial portion of their workday documenting patient visits, updating records, coding procedures, and managing clinical documentation. In many cases, administrative tasks consume nearly as much time as direct patient care. Automation through AI EMR features can dramatically reduce this burden.
Demand for improved patient outcomes
Ultimately, the main goal of integrating AI into EHR platforms is to improve patient outcomes. AI tools can analyze historical patient data to identify early signs of disease, recommend treatment options, and detect potential complications.This is one of the clearest examples of using AI EHR solutions to improve electronic health records in ways that directly benefit both clinicians and patients.
How AI improves EHR
AI can enhance EHR applications in several practical ways. For healthcare providers and software vendors planning AI EHR development, these use cases show how intelligent features can turn traditional record systems into more proactive clinical platforms.
Natural language processing for clinical notes
With natural language processing (NLP), clinicians can simply speak or dictate their notes instead of typing them manually. The system listens, interprets the clinical context, and automatically converts the conversation into structured medical documentation.
Automated data extraction
Healthcare records often contain large amounts of unstructured information such as scanned documents, handwritten notes, or printed medical reports. An intelligent AI EHR system can extract key data from these sources using technologies like optical character recognition and intelligent data parsing.
Once processed, the system can organize the information within the EHR and link it to standardized medical codes.
AI-powered documentation assistance
Many modern EHR solutions include built-in AI assistants that help clinicians manage patient records more efficiently. The system can auto-complete patient information, and surface important details from previous visits (e.g.,recent test results) while the clinician reviews the record.
Diagnostic insights and risk alerts
AI can also support clinical workflows by analyzing patient data and identifying potential health risks. For example, the system may interpret medical images and alert clinicians about patients who may be at risk of serious conditions.
Telehealth and smart scheduling
As telemedicine becomes more common, modern EHR platforms often include tools that support virtual care. AI can assist with appointment scheduling, reminders, follow-ups, and coordinating virtual consultations.
Intelligent billing
AI-powered EHR systems can review clinical documentation, suggest appropriate billing codes, and prepare reports required for insurance claims. Similar capabilities are also driving interest in AI EMR modernization, especially among organizations looking to modernize both electronic medical records and broader digital health workflows.
Barriers to AI adoption in EHR
Integrating Artificial Intelligence into EHR platforms isn't a "plug-and-play" endeavor. While the potential for clinical decision support and administrative automation is massive, the road to implementation is often blocked by systemic technical debt, strict regulatory frameworks, and the simple reality of human skepticism. Moving from a legacy database to an AI-driven ecosystem requires addressing several high-stakes hurdles before the first line of code is even written.
Data privacy and security
EHR applications store highly sensitive patient information. When AI tools analyze this data, healthcare organizations must ensure strict compliance with regulations such as HIPAA and GDPR. Failure to do so puts companies at risk of violating the regulations, which can result in costly fines in addition to negative reputational impacts and loss of patient trust.
Mitigation strategy: implement "Privacy by Design" principles by utilizing data de-identification and anonymization techniques before feeding records into AI models. Additionally, deploying AI within a localized, HIPAA-compliant cloud environment ensures that sensitive PHI (Protected Health Information) never leaves the secure perimeter of the organization.
Interoperability issues
Many hospitals still use legacy healthcare systems that were not designed to support modern AI EHR software. Integrating AI into existing EHR platforms can require major technical upgrades, which can be costly and time-consuming.
Mitigation strategy: adopt Fast Healthcare Interoperability Resources (FHIR) standards to create a universal data language between the legacy EHR and the new AI layer. By using middleware or custom APIs to bridge the gap, you can extract and normalize data for AI processing without needing to overhaul the entire core infrastructure at once.
Bias in AI models
AI systems learn from historical data. If the training data is incomplete or not diverse enough, the AI model may produce biased or inaccurate results. In healthcare, this could affect diagnoses, treatment recommendations, or patient risk predictions.
Mitigation strategy: establish a rigorous data auditing process that screens training sets for demographic gaps. Developers should utilize "Explainable AI" (XAI) frameworks that allow data scientists to trace how a model reached a specific conclusion, making it easier to spot and correct algorithmic bias before the tool reaches the point of care.
Workforce trust and training
Healthcare professionals also need time to adapt to new technologies. Some clinicians may be hesitant to rely on AI tools if they do not fully understand how they work.
Mitigation strategy: involve clinicians early in the UI/UX design phase to ensure the AI output fits naturally into their existing clinical workflow. Providing "Human-in-the-loop" (HITL) systems—where the AI offers suggestions rather than autonomous decisions — empowers doctors to remain the final authority, reducing the friction of adoption.
Real-world examples
Navina is a healthcare AI platform that integrates with major EHR solutions such as Epic, Cerner, and Athenahealth. The platform analyzes patient records in real time and surfaces relevant clinical insights during appointments.
For example, Navina’s AI can:
- flag potential diagnoses
- identify medication conflicts
- highlight patient risk factors
- assist with coding and billing
The system is currently used by over 1,300 clinics, helping physicians quickly interpret complex patient data stored in EHR systems.
Epic has also introduced multiple AI assistants designed for different parts of the healthcare workflow. These include:
- Art – assists clinicians with documentation and decision support
- Emmie – interacts with patients through the MyChart portal
- Penny – supports revenue cycle tasks such as billing and claims management
Early deployments show improvements in documentation speed, earlier diagnoses, and fewer insurance claim denials.
Wrapping up
EHRs solved the problem of paper charts. What they did not solve is how to fully use the data inside them. That is where AI and EHR steps in.
Instead of acting as static databases, an AI EHR system can analyze patient histories, surface important insights, and automate many routine tasks. Of course, the transition is not without challenges, but the shift toward AI EHR solutions is becoming a necessary step toward smarter and more efficient healthcare delivery.








.png)



